Can Extensive Tattoos Make Melanoma Detection More Difficult? Case Report
Main Article Content
Abstract
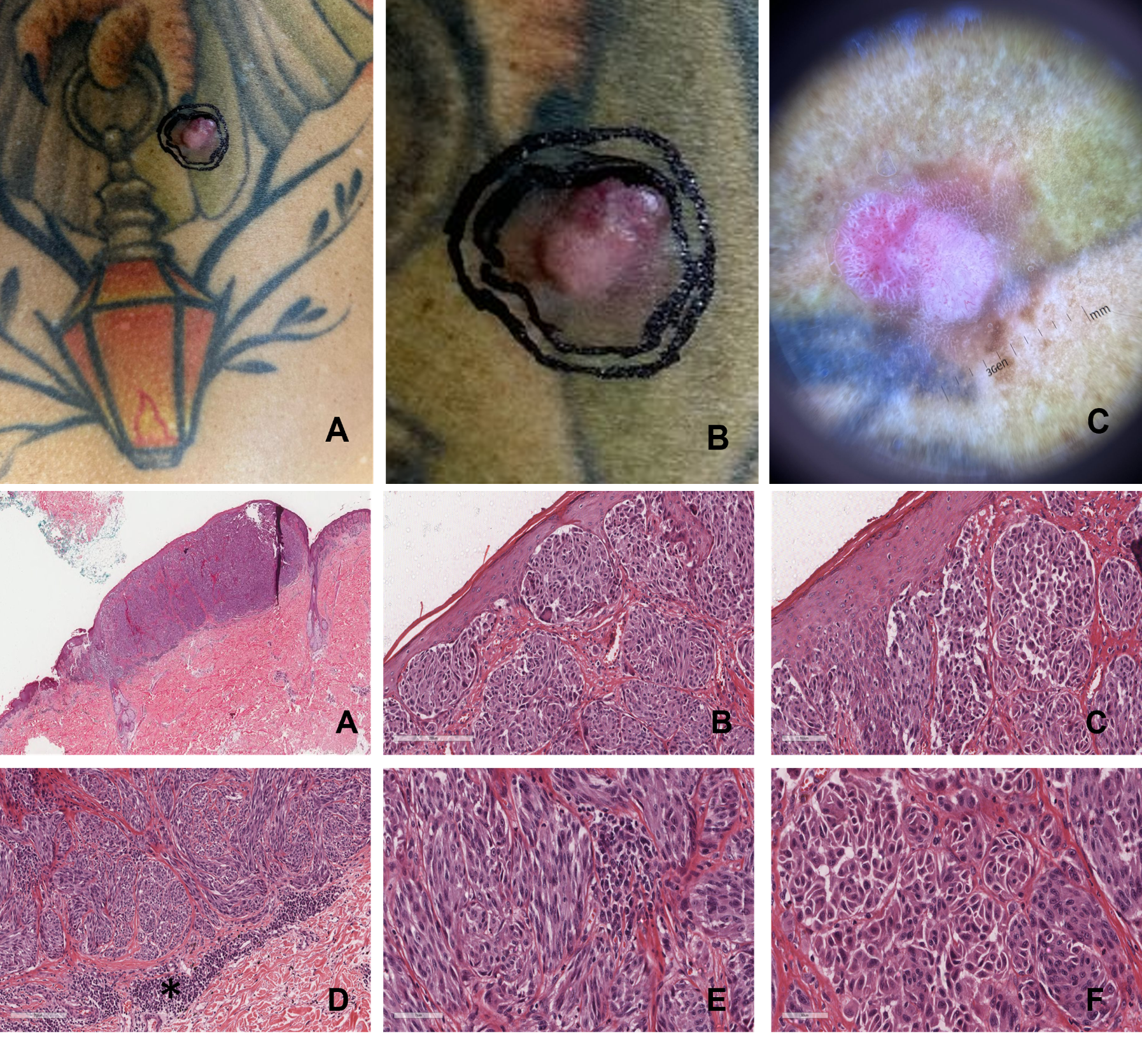
Male patient, 42 years old, skin type I, smoker. He had a lesion on his back for several years, with reports of a nodule appearing on it 6 months ago. The examination revealed a 1.2 cm nodular erythematous violaceous lesion over the right lumbar region of an extensive tattooed area. Dermatoscopy revealed a heterogeneous lesion with flat and nodular components, presenting multiple colors. At the base, there was a brownish, asymmetrical pigmented lesion with an atypical network, inverted network, punctiform vessels, and bright white lines. Over this area, there was an erythematous nodular component with polymorphic vessels and bright white lines, forming a multicomponent pattern. An excisional biopsy with a 2 mm margin was performed, identifying nodular melanoma, Breslow 3 mm.
Article Details

This work is licensed under a Creative Commons Attribution 4.0 International License.
Authors retain the copyright of their articles and grant the journal the right of first publication under the Creative Commons Attribution (CC BY) license, which allows others to share and adapt the work with proper attribution.
References
Brusasco M, Spagnolini S, Mazzoni L, Magi S, Scarcella G, Stanganelli I. Melanoma Arising in Tattoos: A Case Series and Scoping Review of the Literature. Cancers (Basel). 2025;17(5):767. doi:10.3390/cancers17050767.
TATTOOING: Background. Accessed May 29, 2025. https://tattoo.iarc.who.int/background/.
Lallas A, Paschou E, Manoli SM, et al. Dermatoscopy of melanoma according to type, anatomic site and stage. Ital J Dermatol Venerol. 2021;156(3):274-288. doi:10.23736/S2784-8671.20.06784-X.
Menzies SW, Moloney FJ, Byth K, et al. Dermoscopic Evaluation of Nodular Melanoma. JAMA Dermatol. 2013;149(6):699. doi:10.1001/jamadermatol.2013.2466.
Druskovich C, Kelley J, Aubrey J, Palladino L, Wright GP. A Review of Melanoma Subtypes: Genetic and Treatment Consi-derations. Journal of Surgical Oncology. 2025;131(3):356-364. doi:10.1002/jso.27953.
Gronbeck C, Kerr PE. Nodular melanoma. Clin Dermatol. 2025;43(1):64-70. doi:10.1016/j.clindermatol.2025.01.015.
Bobos M. Histopathologic classification and prognostic factors of melanoma: a 2021 update. Ital J Dermatol Venereol. 2021;156(3). doi:10.23736/S2784-8671.21.06958-3.
Shaikh WR, Dusza SW, Weinstock MA, Oliveria SA, Geller AC, Halpern AC. Melanoma Thickness and Survival Trends in the United States, 1989–2009. JNCI: Journal of the National Cancer Institute. 2016;108(1). doi:10.1093/jnci/djv294.